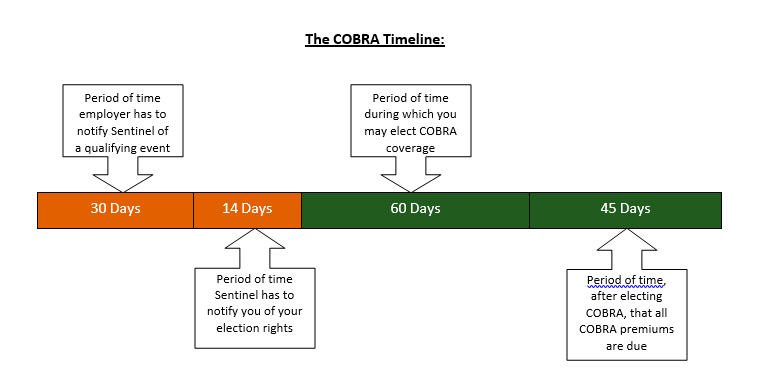
After experiencing a “qualifying event”, you may be eligible to continue your benefits under COBRA. Sentinel Group will be your COBRA administrator. Below is a timeline of how the process will work and important information to keep in mind.
What to know:
- Sentinel will mail COBRA paperwork to your home address within the timeframe noted above. This will have information on your rights and the cost of coverage.You will have a 60 day window to elect COBRA coverage.
- After electing COBRA coverage, your first payment (during the 45 day window) must cover premiums from the date you lost benefits up through the month in which you are paying.
- Active benefits with your employer terminate on your qualifying event date. You must make your benefit elections and payment through COBRA to activate your continued coverage
- Your coverage will not be reinstated until Sentinel receives your first payment.
- Your first payment can be made by check, ACH, or immediate one time payment. Please visit this article for more information on payments: https://help.sentinelgroup.com/help/automatic-payments
- After electing COBRA coverage and making payment, your coverage will be reinstated with the insurance carriers within 5 ‐ 8 business days. The effective date of COBRA coverage will be the date when the original coverage was lost.
- To continue coverage under COBRA, payments are due every month. Sentinel will not send a bill each month. Payments are due on the first day of each month. There is a 30 day grace period in which you can send payment. As long as the payment is postmarked by the last day of the month for which you are paying, the payment will be deemed timely (ex. if you are sending payment for October, the payment will be timely as long as it is postmarked by October 31. ).