If a submitted claim is denied you will receive a notification of denial by email directing you to view the details in your online account.
1. Go to Message Center
Once you are logged into your online account select Message Center from your Main Account page. There will be an indicator that you have new messages. You will need to allow POP-UPS in settings in order to see the letter:
2. Review Claim Notice and Details on Denial
Once in the Message Center, click on the notice associated with your claim. Notifications Associated with claims:
- Request for More Information - Notification will be received when supporting documentation for a Debit Card transaction is provided and additional supporting documentation is required. Additional description and reasons for more information will also be on the letter if necessary. See example here. To upload additional documentation find instructions here.
- Denial Letter - Letter will explain denial reasons and further action required. See example.
- First Receipt Request - Notification received after a debit card transaction that requires additional supporting documentation.
- Overdue Notice - Second notification that additional documentation is required. This notification will be received 2 weeks after the first request is issued.
- Ineligible Notice - Notification received if:
- Documentation was received and the item is not eligible for reimbursement. If the item was purchased using the debit card, the card will be suspended and the amount of the charge needs to be repaid to the plan. Please see instructions for repayment. Note: The participant can file claims to offset a repayment but you would need to submit a ticket to Flex to notify them of this AND add a comment when submitting their new reimbursement request that they would like to offset the repayment for a specific claim. In this case the repayment amount would either decrease, be wiped out (if exactly the same amount), or the reimbursement amount will be the approved claim submission minus the repayment amount.
- Previous requests for documentation received no response. In this case, the transaction will be deemed ineligible and the debit card will be suspended.
3. Upload additional documentation
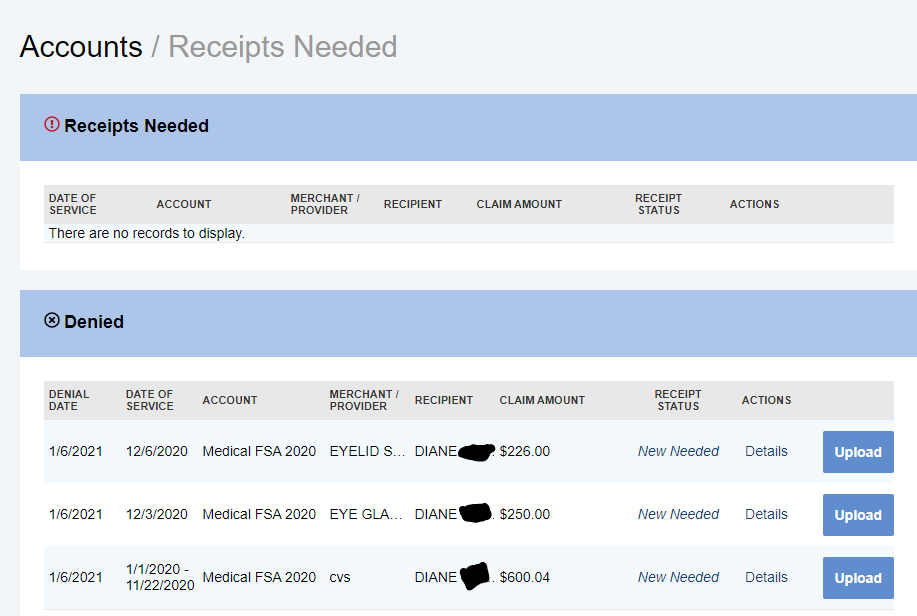
When a claim requires additional information to be approved you will be prompted on your home screen to upload additional documentation (max 4 documents). Click on the link to view all of the claims for which you need to submit a receipt.
- In the receipts page you will be able to view additional details about the claim by clicking the Details link then View Denial to see details. To upload requested documentation Click on the Upload button
When uploading documentation please be aware of the system limitations and format of document accepted. 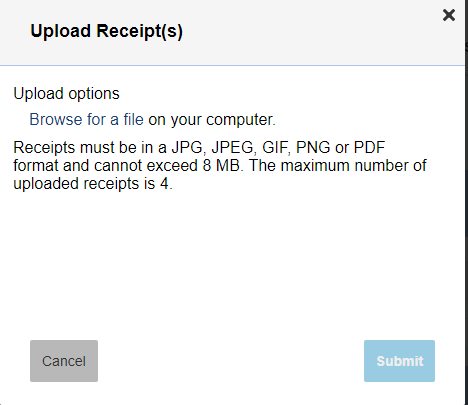
4. Acceptable Documentation
In order for your claim to be in good order there is specific detail that is required.
Medical FSA: The Explanation of Benefits (EOB) from insurance provider will have all of the needed information above. If you do not have your EOB you may also provide receipt directly from provider.
YES | NO |
Required Details:
 | Credit Card receipt does not contain sufficient detail to show services received. (*exception: Pharmacy receipt is acceptable documentation for Rx purchases)  |
Please Note - If you are not able, or prefer not to upload your receipts online, you may print the confirmation page and send to Sentinel Group by Fax: 781-213-7301 Email: Customer Service or Mail: 100 Quannapowitt Parkway Suite 402 Wakefield, MA 01880
Still have questions or issues with updating claims? Contact Us